One of the most common problems leading patients to seek medical attention is neck or back pain. This is because most of the motion of the spine occurs in the neck (cervical spine) or the back (lumbar spine). Often, patients who seek help may end up confused when they are told they have “degeneration” or “arthritis” when imaging reports list disc bulges and osteophytes, or spurs.
Anatomy
A disc is the “cushion” between two vertebrae (or bones) in the spine. Whether cervical or lumbar, it has the same structure and function – it serves as both a shock absorber as well as helps with motion and stability of the spine. A useful analogy is to think of the disc as a tire on its side. The outer portion of the disc is similar to multiple layers of the tire while the inner portion of disc is like the air in the tire. When the tire is properly inflated the walls are under tension and provide strength and stability while still being able to flex. As the tire gets low on air, the walls are under less tension to bulge out, providing less stability and allow wobbling.
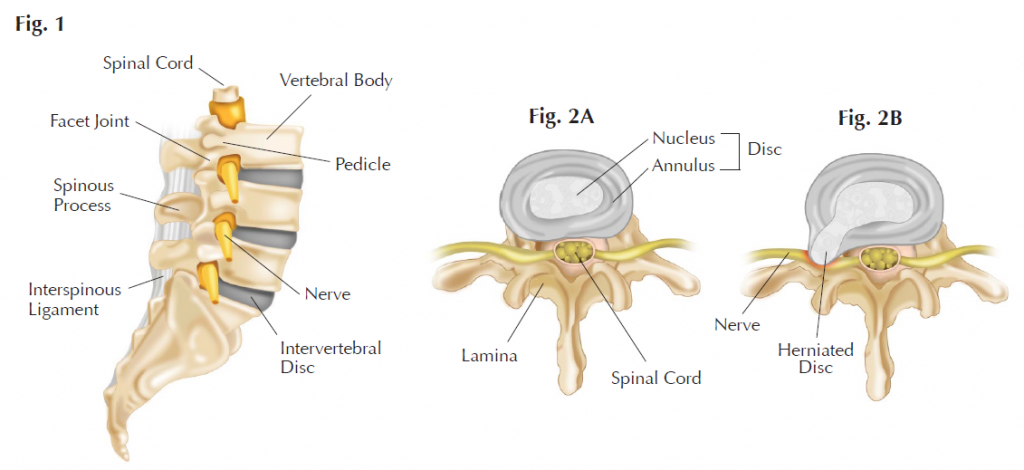
The disc is very similar. When we are younger, the disc is similar to a properly inflated tire. The inner portion of the disc is hydrated and strong, and it keeps the outer portion of the disc under tension. Movement is allowed, but it is stable. As we age (typically in the twenties) the inner portion of the disc starts to dry out, providing less tension on the outer portion of the disc. The disc may bulge and not be as stable or strong. As more aging occurs, the disc may actually look shorter in height, with less water content. The body tries to compensate, and eventually spurs form in an attempt to stabilize the region.
These changes are referred to as spinal spondylosis and are best seen on MRI imaging. The same change may also be called “degenerative disc disease”, “degeneration”, or “arthritis” by some doctors. However, what gets confusing is that all of these changes are part of the natural aging process, not any disease.
Causes of Pain & When to Seek Treatment
If you are having neck pain or back pain, it could just be a muscle or fascia strain. However, pain, numbness or weakness in the arm or leg could be a more serious issue, such as a bulged disc (also called a herniation or extrusion) or a bone spur pressing on a nerve or the spinal cord. On the other hand, sometimes what is thought to be a spinal issue may actually be a hip or shoulder issue, or simply carpal tunnel syndrome. Since the source of neck and back pain can vary, it’s important to consider seeing a specialist for evaluation. After reviewing your medical history, performing a physical exam, and ordering any necessary tests (e.g. MRI), a specialist can help determine the best course of action, including but not limited to therapy, injections or surgery.
Minimally Invasive Surgery
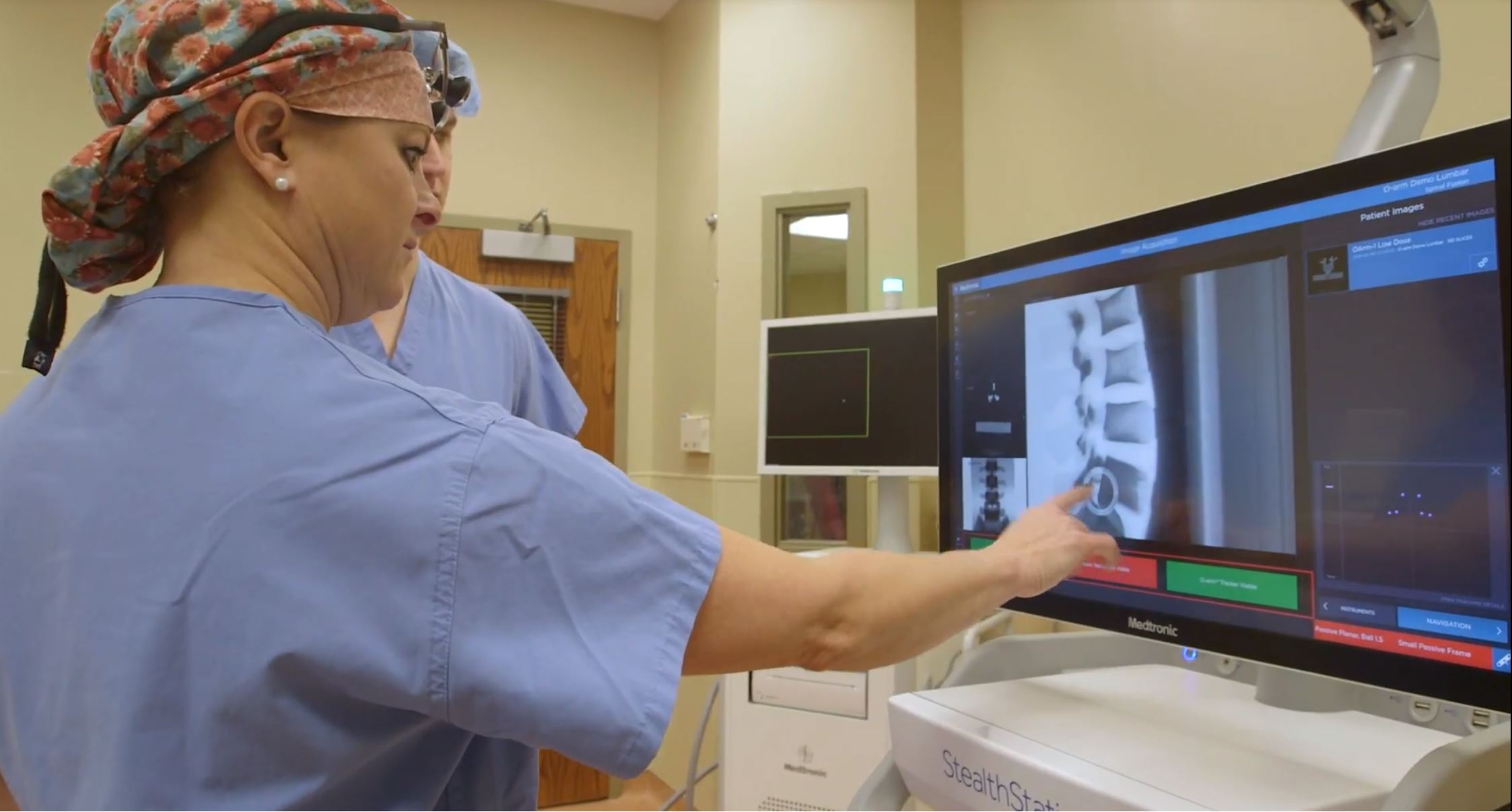
Should surgery be the best course of action, there are minimally invasive procedures available, sometimes performed in an outpatient setting. Minimally invasive spine surgery allows the surgeon to make much smaller incisions in the skin and avoid any unnecessary muscle damage, while achieving the same surgical result. Muscle is left intact and only separated, or “split,” along natural divisions to reach the affected area. Special live-action x-ray machines are used along with imaging systems and tiny cameras (image guidance or navigation), so a large opening isn’t needed to visualize the problem. Orthopedic surgeons and neurosurgeons can then work precisely through the smaller openings, which mean significantly less tissue trauma to the patient. Spinal fusion and cervical disc arthroscopy are two procedures that can be performed using minimally invasive approaches.
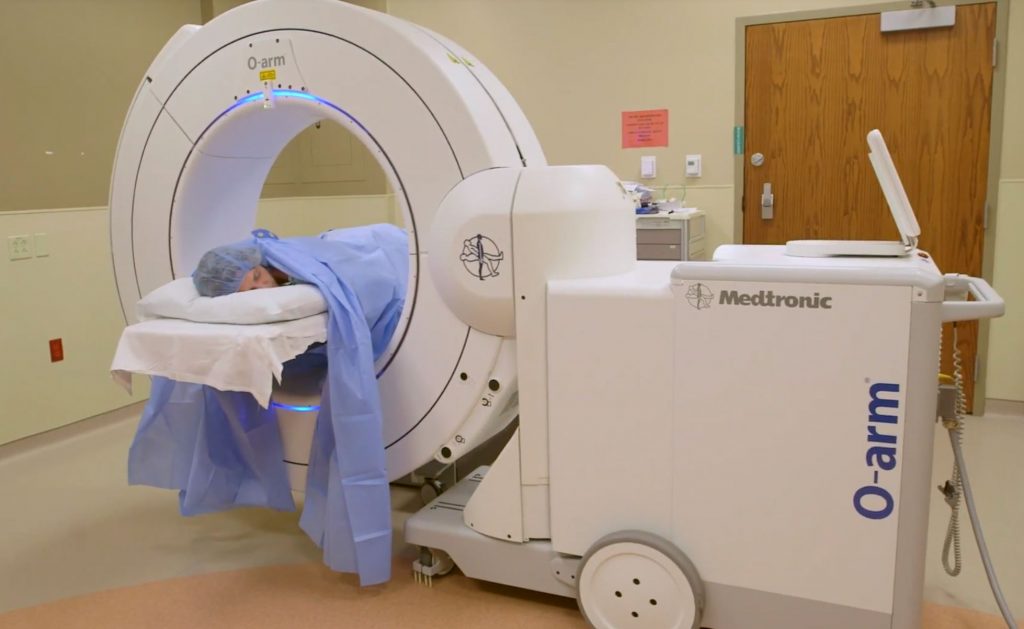
(O-arm™ surgical imaging system used during minimally-invasive spine surgery)
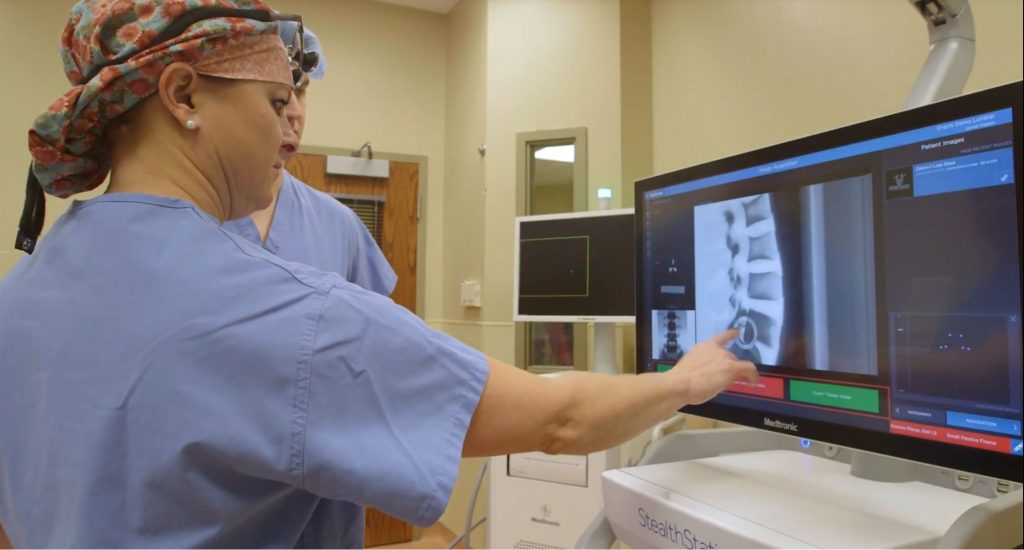
(Dr. Tekula using StealthStation™ navigation (part of the O-arm system), which provides enhanced visibility of the spine during surgery.)
Advantages of minimally invasive procedures include:
- Recovery is faster with less post-operative pain
- Quicker return to work and normal activities
- Shorter hospital stays – outpatient surgery vs. two to three days with open surgery
- Less soft tissue damage, due to reduced muscle stripping (retraction)
- Incisions are much smaller (less than one inch vs. up to four inches) so scarring is less noticeable
- Reduced blood loss
In conclusion, there are many different causes of neck and back pain. If the discomfort is too great and/or the issue persists, it is likely time to make an appointment with a specialist for evaluation. A specialist can work to find the source of the pain and help determine the best course of action for pain relief. Should surgery be needed, minimally invasive procedures are available, sometimes in an outpatient setting.